Introduction
Retatrutide is a triple-receptor agonist; it activates GLP-1, GIP, and glucagon receptors simultaneously. It comes as a freeze-dried powder inside a sealed vial. Before each injection, you mix the powder with bacteriostatic water (BAC water) to create a liquid solution. The dose you then inject depends entirely on two things: how much BAC water you added and which syringe you use. A retatrutide dosage calculator takes the guesswork out of this process.
Unlike a tablet or a pre-dosed pen, retatrutide requires you to work through four unit conversions every time you prepare a dose. The vial is labelled in milligrams (mg). The calculation runs through micrograms (mcg) and millilitres (mL). The final answer is a number on the barrel of an insulin syringe.
This guide explains exactly how that calculation works. It covers the core formulas in plain English, shows worked examples, and explains how to use a retatrutide dosing calculator step by step. You will also find the standard titration schedule, a comparison of retatrutide with other GLP-1 medications, a list of common mistakes, and an FAQ section.
Retatrutide is not FDA-approved. It is currently in Phase 3 clinical trials under the name TRIUMPH-1, developed by Eli Lilly. Always work with a licensed healthcare provider before using or adjusting any investigational medication.
| Key Takeaway: This guide covers: the exact dosage calculation math, a step-by-step guide to using a retatrutide dosing calculator, the titration schedule from Phase 2 and Phase 3 trial data, and answers to the most common questions about retatrutide dosing. |
What Is a Retatrutide Dosing Calculator?
Definition
A retatrutide dosing calculator is an online tool that converts your vial size (mg), your BAC water volume (mL), and your target dose (mg or mcg) into the exact number of syringe units to draw. It handles all four unit conversions automatically. You put in three numbers, and you get back one clear answer.
There are two types of retatrutide calculators:
- The reconstitution calculator tells you the concentration (mcg per mL) after you mix your vial. This is the first step in any dose preparation.
- The full dosing calculator goes further. It adds the draw volume (mL) and the exact syringe units, plus the total number of doses in the vial.
Most people need a full dosing calculator. The reconstitution calculator alone does not tell you how much to draw.
Why Do You Need One?
Retatrutide dosing is not like taking a tablet. The dose changes every time anything about your preparation changes. If you add more BAC water than usual, your concentration drops. That means a different draw volume and different syringe units, even for the same prescribed dose.
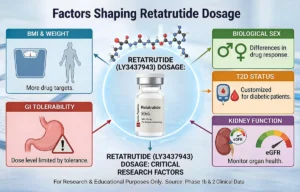
Beyond preparation variables, the target dose itself may differ by participant factors like BMI, sex, diabetes status, and kidney function, all of which play a role, as explained in the 8 key retatrutide dose factors in clinical studies.
Manual conversion errors are the most common problem. The four-step conversion mg to mcg, then concentration, then draw volume, then syringe units- gives four chances for a mistake. A single wrong entry can send the calculation in the wrong direction by a factor of 1,000.
The main risks of getting this wrong are wasted product, inconsistent results, and, in some cases, a dose that is much too high or too low. A retatrutide dosing calculator removes all of that risk. It is not optional; it is the safest way to prepare each dose.
| ! One vial, many possible doses. The same 10 mg vial can produce very different concentrations depending on how much BAC water you add. Adding 1 mL gives a concentration of 10,000 mcg/mL. Adding 3 mL gives 3,333 mcg/mL. The dose volume is different every time. A retatrutide dosing calculator keeps this accurate. |
How Retatrutide Dosage Calculation Really Works
The retatrutide dosage calculation follows five clear steps. Each step builds on the last. Once you understand the logic, the calculator makes perfect sense.
Step 1: Understand the Units
Before you enter anything into a calculator, you need to know what each unit means.
| Unit | What it measures | Where you see it |
|---|---|---|
| mg (milligram) | Mass of the peptide | Vial label (e.g. 10 mg, 20 mg) |
| mcg (microgram) | 1 mg = 1,000 mcg | Calculator does input fields |
| mL (millilitre) | Volume of liquid to draw | Syringe barrel markings |
| Units (U-100) | Syringe markings, 100 units = 1 mL | U-100 insulin syringe scale |
The most important conversion to memorise: 1 mg = 1,000 mcg.
This is where most calculation errors happen. Your vial is labelled in mg. Your calculator may ask for the dose in mcg. Always check which unit each input field expects before you type a number.
On a U-100 insulin syringe: 100 units = 1 mL. So 50 units = 0.5 mL and 20 units = 0.2 mL. This conversion bridges concentration (mcg/mL) and the syringe scale (units).
Step 2: Reconstitute Your Vial, The Concentration Formula
Reconstitution means adding BAC water to the freeze-dried powder in your vial to create an injectable solution. The amount of BAC water you add determines the concentration of the solution.
| Formula: Concentration (mcg/mL) = Vial mg × 1,000 ÷ BAC water mL In plain English: Multiply the vial size by 1,000 to convert to mcg, then divide by the number of mL of BAC water you added. |
Here is how this plays out with a standard 10 mg vial:
| BAC Water Added | Concentration | What this means for your dose |
|---|---|---|
| 1 mL | 10,000 mcg/mL | Very concentrated. Very small draw volumes. Harder to measure small doses accurately. |
| 2 mL | 5,000 mcg/mL | Standard choice. Comfortable draw volumes for most dose sizes. |
| 3 mL | 3,333 mcg/mL | More dilute. Larger draw volumes. Easier to measure lower doses precisely. |
Adding more BAC water does not change how much retatrutide is in the vial. It only spreads the same amount across a larger volume. More water means a lower concentration, which means a larger liquid volume per dose. For lower doses, such as 1 mg or 2 mg early in the titration schedule, a more dilute solution is easier to measure accurately.
| ✓ Always use bacteriostatic water (BAC water). BAC water contains a preservative called benzyl alcohol that stops bacterial growth. Sterile water contains no preservative and is safe for single use only. Because you draw from a retatrutide vial multiple times, bacteriostatic water is always the correct choice. Never use tap water, saline, or sterile water for multi-dose peptide vials. |
How to mix your vial correctly:
- Allow the peptide vial and BAC water to sit until they reach room temperature.
- Wipe the top of each vial with a fresh alcohol swab.
- Draw your chosen BAC water volume into a sterile syringe.
- Insert the needle into the peptide vial and inject the water slowly down the inside wall — never directly onto the powder.
- Gently swirl the vial. Never shake it. Shaking can damage the peptide.
- Check that the powder has fully dissolved. The final mixture should appear transparent and free of any colour.
- Keep the mixed vial refrigerated at 36–46°F (2–8°C). Discard after 28–60 days.
Step 3: Calculate Your Draw Volume
Once you have your concentration, calculating the draw volume is one simple division.
| Formula: Draw volume (mL) = Desired dose (mcg) ÷ Concentration (mcg/mL). In plain English: Divide the dose you need (in mcg) by the concentration of your solution (in mcg/mL). |
Worked example: 10 mg vial + 2 mL BAC water → concentration = 5,000 mcg/mL. For a 2 mg dose (2,000 mcg): 2,000 ÷ 5,000 = 0.40 mL.
Step 4: Convert Draw Volume to Syringe Units
The final step converts your draw volume in mL into the unit mark you pull the syringe plunger to.
| Formula: Syringe units = Draw volume (mL) × 100 In plain English: Multiply mL by 100 to get the unit mark on a U-100 insulin syringe. |
Continuing the example: 0.40 mL × 100 = 40 units. Pull the plunger to the 40-unit mark on your U-100 syringe.
Below is a full reference table for a 10 mg vial reconstituted with 2 mL of BAC water. This gives a concentration of 5,000 mcg/mL.
| Dose (mg) | Dose (mcg) | Draw Volume (mL) | Syringe Units, U-100 |
|---|---|---|---|
| 1 mg | 1,000 mcg | 0.20 mL | 20 units |
| 2 mg | 2,000 mcg | 0.40 mL | 40 units |
| 4 mg | 4,000 mcg | 0.80 mL | 80 units |
| 8 mg | 8,000 mcg | 1.60 mL | 160 units, use 2 separate injections |
| 12 mg | 12,000 mcg | 2.40 mL | 240 units, use 3 separate injections |
If you use a different vial size or a different BAC water volume, your concentration changes, and so do all the numbers in this table. Run the calculation again every time anything about your preparation changes.
Step 5: Verify Total Doses Per Vial
Knowing how many full doses your vial contains helps you plan your supply and avoid running short.
| Formula: Total doses = (Vial mg × 1,000) ÷ Dose mcg, then round DOWN. In plain English: Divide the total peptide in the vial (converted to mcg) by your dose in mcg. Always round the result down, never up. |
Example: 10 mg vial, weekly dose of 2 mg (2,000 mcg). → 10,000 ÷ 2,000 = 5 doses per vial.
If the math gives you 5.8, you have 5 complete doses. The 0.8 is not a full dose and should not be counted.

How to Use a Retatrutide Dosing Calculator Step by Step
A retatrutide dosing calculator does all five steps above in under a second. The following steps explain how to use it properly.
Inputs You Will Need
Every retatrutide dosing calculator asks for the same four pieces of information:
| Input field | What to enter | Example |
|---|---|---|
| Vial size | Total peptide in your vial, in mg, not mcg | 10 mg |
| BAC water | Volume of bacteriostatic water you are adding, in mL | 2 mL |
| Target dose | The dose your provider prescribed, in mg or mcg | 2 mg or 2,000 mcg |
| Syringe size | The maximum capacity of your insulin syringe | 0.5 mL or 1.0 mL |
Outputs You Will Get
Once you enter those four values, the retatrutide dosing calculator gives you:
- Final concentration in mcg/mL, the strength of your mixed solution
- Dose volume in mL, how much liquid to draw
- Syringe units, the exact mark on the barrel to pull to
- Total doses per vial: how many full injections can you get from this vial
Step-by-Step: Using the Calculator
- Open a reliable retatrutide dosing calculator, preferably one recommended by your provider or clinic.
- Enter your vial size in milligrams (mg). If your vial says 10 mg, enter 10, not 10,000.
- Enter the BAC water volume in mL, the amount you plan to add during reconstitution.
- Enter your target dose. Check whether the field expects mg or mcg. Input the value using the correct unit.
- Select your syringe size (0.3 mL, 0.5 mL, or 1.0 mL).
- Read the output. The syringe unit’s field tells you exactly where to pull the plunger to.
- Recalculate every time you open a new vial, change your BAC water volume, or receive a new dose from your provider.
| ! Most common calculator mistake Entering the vial size in mcg instead of mg. If your vial is 10 mg and you type 10,000 thinking it is in mcg, the calculator will calculate a dose 1,000 times larger than intended. Always confirm: the vial size field takes milligrams (mg). |
Retatrutide Titration Schedule: What Doses to Calculate For
Retatrutide starts at 1–2 mg once weekly and increases every 4 weeks to a maximum of 12 mg.
This gradual dose increase is called titration. It gives your body time to adjust to the medication and reduces side effects such as nausea. The schedule below is based on Phase 2 clinical trial data and the TRIUMPH-1 Phase 3 trial.
| Weeks | Weekly Dose | Clinical Source | What to expect |
|---|---|---|---|
| Weeks 1–4 | 1 mg or 2 mg | Phase 2 trial/clinic protocol | Appetite begins to decrease. You may feel fuller more easily. |
| Weeks 5–8 | 2 mg or 4 mg | Phase 2 trial | Appetite control becomes more consistent. First weight changes often appear. |
| Weeks 9–12 | 4 mg | Phase 2 trial | Stronger appetite suppression. Side effects typically stabilise. |
| Weeks 13–16 | 8 mg | Phase 2 trial | Significant appetite reduction for most people. |
| Week 17+ | 8 mg or 12 mg (max) | Phase 2 / TRIUMPH-1 trial | 12 mg is the maximum dose. Not everyone needs the highest level. |
Dose escalation is not automatic. Your provider adjusts the schedule based on how your body responds. If side effects are significant, they may keep you on the current dose for another 4 weeks before increasing. A slower titration is completely normal and often leads to better long-term results.
Why the 4-Week Interval Matters
Retatrutide stays active in the body for about six days due to its half-life. After you inject a dose, the medication stays active in your body for nearly a week. After 4 to 5 weeks of consistent dosing at the same level, the drug reaches what is called steady state, where the concentration in your blood stabilises and becomes predictable between injections.
You cannot accurately assess whether a dose is working until it has reached steady state. Moving up too fast means you are making decisions based on levels that are still rising. This is why the titration schedule uses 4-week intervals, not shorter ones.
Why the Calculator Is Especially Important During Titration
Every time your dose changes, the syringe units change. If you step up from 2 mg to 4 mg, the calculator gives a completely different number. You cannot use last week’s syringe units with this week’s dose.
Some people also choose to split their weekly dose into two smaller injections, a practice called microdosing. For example, an 8 mg weekly dose might become two injections of 4 mg, taken a few days apart. This aims to keep drug levels more stable. If you split your dose, the calculator needs to reflect the per-injection amount, not the weekly total.
| ✓ Clinical trial weight loss results. In Phase 2 trials, people using retatrutide at higher doses (8 mg and 12 mg) lost an average of 17.5% of body weight after 24 weeks and 24.2% after 48 weeks. The highest doses consistently produced the greatest weight loss, but only when reached gradually and tolerated well. |
Retatrutide vs Other GLP-1 Medications, Dosing Comparison
To use a retatrutide dosing calculator correctly, it helps to understand how retatrutide differs from other GLP-1 medications in terms of dosing structure. The table below compares retatrutide with tirzepatide and semaglutide, the two most widely used GLP-1 class medications as of 2026.
| Feature | Retatrutide | Tirzepatide | Semaglutide |
|---|---|---|---|
| Receptors targeted | GLP-1 + GIP + Glucagon | GLP-1 + GIP | GLP-1 only |
| Common name | LY3437943 (Eli Lilly) | Mounjaro / Zepbound | Ozempic / Wegovy |
| Starting dose | 1–2 mg once weekly | 2.5 mg once weekly | 0.25 mg once weekly |
| Maximum dose | 12 mg once weekly | 15 mg once weekly | 2.4 mg once weekly |
| Dose frequency | Once weekly | Once weekly | Once weekly |
| Needs reconstitution? | Yes, compounded vial | No, pen device | No, pen device |
| Calculator required? | Yes | No | No |
| FDA approval status | Phase 3, not approved | FDA-approved | FDA-approved |
The key difference is clear: retatrutide comes in a compounded vial form and must be reconstituted before each injection. Tirzepatide and semaglutide come as pre-dosed pen injectors, no mixing, no calculation. This is exactly why a retatrutide dosing calculator is essential for retatrutide but not needed for the other two.
Retatrutide’s triple-receptor mechanism targeting GLP-1, GIP, and glucagon simultaneously is also why its dosing scale is different. The glucagon receptor activation increases energy expenditure, which adds a metabolic effect on top of the appetite suppression from GLP-1 and GIP. This combined action is thought to explain the strong weight loss results seen in clinical trials.
6 Common Retatrutide Dosing Calculation Mistakes, And How to Avoid Them
Mistake 1: Confusing mg and mcg
Entering the vial size in mcg instead of mg is the most dangerous mistake. If your vial is 10 mg and you type 10,000 in a field expecting mg, the calculator interprets it as 10,000 mg, one million times the actual amount. The resulting syringe units will be wildly wrong. Always double-check the unit each field expects before entering a number.
Mistake 2: Choosing sterile water instead of bacteriostatic water
Sterile water contains no preservative. It is only safe for a single injection. If you use sterile water in a multi-dose vial, the solution is at risk of bacterial contamination from the second draw onwards. Always use bacteriostatic water (BAC water) for retatrutide reconstitution.
Mistake 3: Not Recalculating After Changing the BAC Water Volume
Your concentration is tied directly to how much BAC water you add. Change the water volume even slightly, and the concentration changes. That means the syringe units change, too. Recalculate using the retatrutide dosing calculator every time you change your preparation.
Mistake 4: Rounding Up Total Doses Per Vial
If the formula gives you 5.8 doses, you have 5 usable doses, not 6. The last 0.8 of a dose is typically not a full, measurable amount. Rounding up leads to drawing from a nearly empty vial, which increases the risk of an underdose or an air bubble. Always round down.
Mistake 5: Syringe Too Small for the Dose
A 0.3 mL syringe holds only 30 units. If your calculated dose is 80 units (0.80 mL), you cannot draw it in one go with that syringe. Always check your calculated draw volume against your syringe size before preparing the injection. For doses of 4 mg and above at standard concentrations, a 1 mL (100-unit) syringe is usually required.
Mistake 6: Evaluating the Dose Before Steady State
Retatrutide takes 4 to 5 weeks to reach stable blood levels at any given dose. Judging whether a dose is ‘working’ before steady state is reached means deciding on incomplete information. Give each dose level the full 4-week interval before discussing any changes with your provider.
FAQ: Retatrutide Dosing Calculator
The questions below are among the most commonly searched queries on retatrutide dosing. Each answer is written to stand alone as a complete, accurate response.
What is a retatrutide dosing calculator?
A retatrutide dosing calculator is an online tool that calculates the exact syringe draw volume for your retatrutide dose. You enter your vial size, BAC water volume, and target dose, and the calculator returns the concentration, draw volume in mL, syringe units, and total doses per vial. It eliminates the need for manual mg-to-mcg-to-mL conversions and the errors that come with them.
How much BAC water do I add to a 10 mg retatrutide vial?
There is no single required amount. It depends on the dose you need and what is easiest for you to measure accurately. Adding 2 mL gives a concentration of 5,000 mcg/mL; 20 units on a U-100 syringe equals 1 mg. Adding 1 mL gives 10,000 mcg/mL; 10 units equals 1 mg. Adding 3 mL gives 3,333 mcg/mL. Use a retatrutide reconstitution calculator to find the right ratio for your specific dose and syringe.
What is the starting dose of retatrutide?
Most clinical protocols begin at 1 mg or 2 mg once weekly. Some providers start at 1 mg for 4 weeks before increasing. This low starting dose gives the body time to adjust to the medication and reduces side effects such as nausea and fatigue. Based on Phase 2 trial data, dose escalation happens every 4 weeks up to a maximum of 12 mg weekly.
What is the maximum dose of retatrutide?
The maximum dose studied in both Phase 2 and Phase 3 (TRIUMPH-1) trials is 12 mg once weekly. No dose above 12 mg per week should be used. Not everyone needs the maximum dose; many people achieve significant weight loss at 8 mg weekly. Your provider will determine the appropriate maintenance dose based on your response and tolerance.
How do I convert retatrutide mg to mcg?
Multiply by 1,000. For example: 1 mg = 1,000 mcg. 2 mg = 2,000 mcg. 8 mg = 8,000 mcg. 12 mg = 12,000 mcg. This conversion is necessary because retatrutide dosing calculators often ask for the desired dose in micrograms (mcg), while vial labels and prescriptions use milligrams (mg).
How many syringe units are 2 mg of retatrutide?
It depends on your reconstitution. If you have a 10 mg vial and add 2 mL of BAC water, the concentration is 5,000 mcg/mL. A 2 mg dose (2,000 mcg) requires 0.40 mL, which is 40 units on a U-100 insulin syringe. If you change your BAC water volume, the concentration changes, and so do the units. Always run the full calculation or use a retatrutide dosing calculator to confirm.
Does retatrutide need to be refrigerated after reconstitution?
Yes. Once mixed with BAC water, reconstituted retatrutide should be stored in the refrigerator at 36–46°F (2–8°C). It is typically stable for 28 to 60 days, depending on storage conditions. Never freeze reconstituted retatrutide. Before each injection, check the solution; if it looks cloudy, discoloured, or contains visible particles, discard it and prepare a fresh vial.
Is retatrutide FDA-approved?
No. As of April 2026, retatrutide is not FDA-approved. It is developed by Eli Lilly and is currently in Phase 3 clinical trials under the TRIUMPH-1 programme. FDA approval is expected in 2026 or 2027. Retatrutide is currently available only through licensed compounding pharmacies under a provider’s supervision, or through approved clinical trial sites. Never use retatrutide without working with a qualified healthcare professional.
Conclusion and Next Steps
Retatrutide dosage calculation follows three formulas. First, multiply your vial size in mg by 1,000, then divide by your BAC water volume in mL to get the concentration in mcg/mL. Second: divide your target dose in mcg by that concentration to get the draw volume in mL. Third: multiply the draw volume by 100 to convert to syringe units for a U-100 insulin syringe. A retatrutide dosing calculator runs all three steps instantly and eliminates the risk of manual conversion errors.
Every time you open a new vial, change your BAC water volume, or receive a new prescribed dose, recalculate. The syringe units change every time the preparation changes. Using the calculator consistently is the single most important habit for accurate, safe retatrutide dosing.
Retatrutide is a powerful investigational triple-receptor agonist with strong clinical results. But those results depend on accurate dosing. Take the calculation seriously. Use the calculator. And always confirm your protocol with a licensed healthcare provider before making any changes.
| Key Takeaway: Use a retatrutide dosing calculator for every preparation. Recalculate every time anything changes. Never guess. |
Reference
- Jastreboff, A. M., Aronne, L. J., Ahmad, N. N., et al. (2023). Triple-hormone receptor agonist retatrutide in obesity without diabetes. The New England Journal of Medicine, 389(6), 514–526.
- Jastreboff, A. M., et al. (2022). Tirzepatide once weekly for the treatment of obesity. The New England Journal of Medicine, 387(3), 205–216.
- Wilding, J. P. H., et al. (2021). Once-weekly semaglutide in adults with overweight or obesity. The New England Journal of Medicine, 384(11), 989–1002.
- Drucker, D. J. (2021). Mechanisms of action of glucagon-like peptide-1. Cell Metabolism, 33(4), 740–756.





 Sign In to Google
Sign In to Google